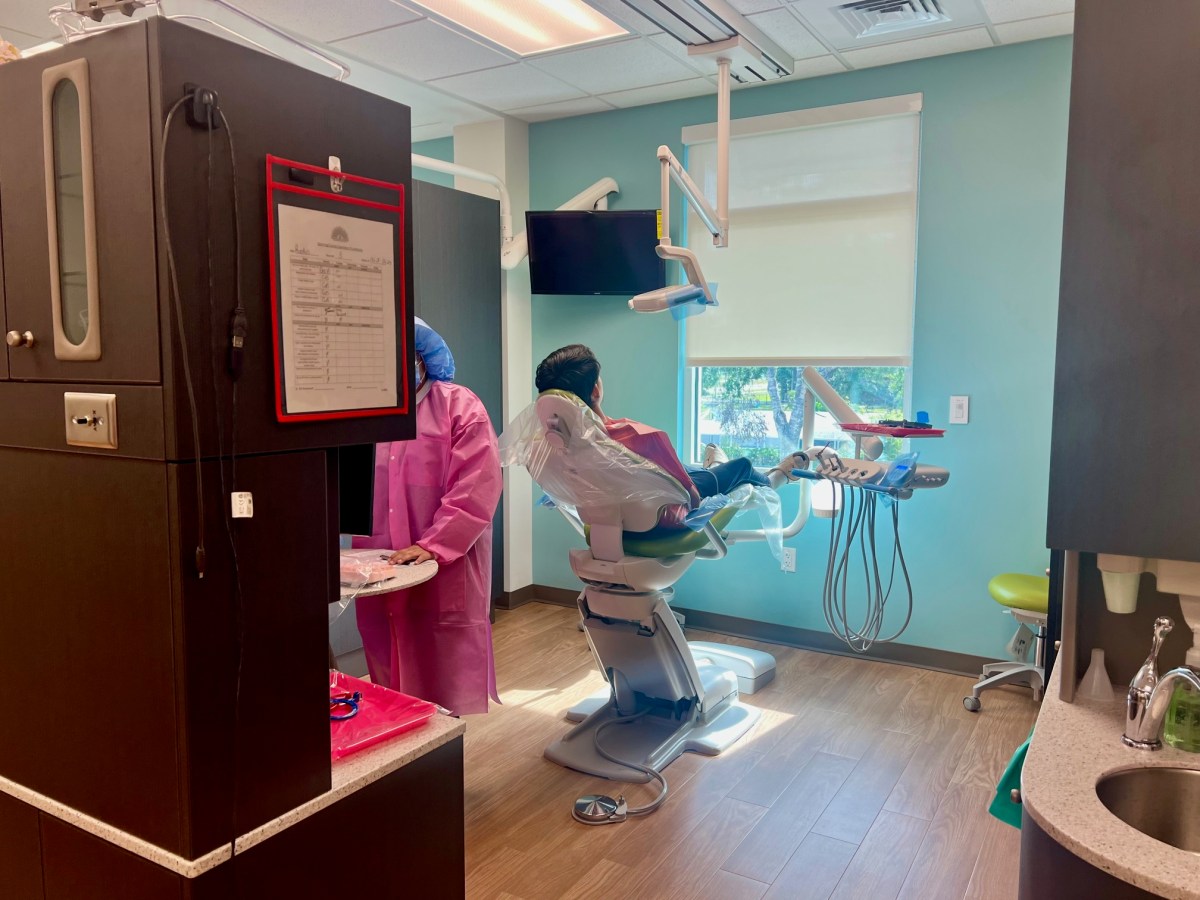
Mornings are always busy at Suncoast Community Health Center’s pediatric dental clinic in Brandon, a community near Tampa. Hallways buzz with sounds of drills and suction tubes as dentists assure kids, “You’re doing awesome,” or, “It will be over soon.”
Patients come to the clinic for the usual teeth cleanings or filling cavities. Then there are severe cases.
“We’ve had children who are three, four or five years old and we’re extracting, pulling, 16 of their 20 teeth due to cavities, the extent of cavities,” said Dr. Tianna Wallick, a second-year pediatric resident at the clinic.
If they have insurance, kids with that much damage may get referred to a hospital for surgery under anesthesia. But for those who don’t have coverage, Wallick said dentists have to make tough choices to get children treatment they need in a way their family can afford.
“We have to do it [extractions] with them awake, with a protective blanket. That is a treatment that hurts my soul – I know they need it, but it hurts my soul,” she said.
WUSF Radio Report:
How Florida’s Fluoride Ban Could Impact Kids
Those are last-resort situations that Wallick said could be avoided if kids had better access to affordable dental care and preventive cleanings, as Suncast offers. But in a state where nearly all counties don’t have enough dentists to meet demand, low-income families have limited options.
For decades, kids who haven’t had access to regular dental care had at least one line of defense against cavities: drinking water with fluoride in it.
But a new state law bans communities from adding the mineral to water supplies. Some dentists warn the ban, which takes effect July 1, will take away an important tool that kids in poor and rural areas depend on to prevent tooth decay.
“Prevention is more important than anything else,” said Dr. Aura Cisneros, chief dental officer at Suncoast. “Once you need to treat the problem, it’s already too late.”

Millions live in ‘dental deserts’
Nearly 6 million residents in the state live in what the federal government designates as dental health professional shortage areas. Most dentists who do practice in Florida aren’t regularly treating patients with low incomes because they don’t accept Medicaid or their prices are well beyond what these individuals can afford.
County health departments and community health centers like Suncoast serve as critical safety nets, but a significant number of children still live with untreated problems.
“Most of the time when they come to us, it’s like the end of the road,” said Cisneros said.
The group provides care at clinics in rural and suburban Hillsborough County. It also operates a mobile dental program to provide routine care in schools and family resource centers.
Many children who visit are on Medicaid, but Suncoast also treats a lot of immigrants who don’t have legal status, Cisneros said. Unlike some other states, Florida does not allow these children to qualify for Medicaid, so families must pay out-of-pocket for care.
“Here, we have the opportunity to bring the best quality care possible for everybody seeking help, and we can make a difference in their life,” Cisneros said.
As a community health center, Suncoast gets federal money to treat Medicaid patients and offer discounted care to people without insurance — as low as $25 for a routine visit.
It’s a huge help for parents like Santiago Gomez. On a recent morning in late April, Gomez said his 5-year-old son’s Medicaid insurance would pay for the stainless steel crowns he needed — and for sedation during treatment.
But Gomez said finding a place to accept that coverage was difficult.
“I’m frustrated,” he said in Spanish. “Because we don’t know what’s going on with his teeth, but I imagine he must be in pain all the time.”

Nearly 80% of Florida dentists don’t take Medicaid, according to the most recent dental workforce survey published by the Florida Department of Health. The vast majority of respondents cited “inadequate reimbursement” as the main reason.
The state’s reimbursement rates are among the lowest in the nation. The American Dental Association estimates Florida’s Medicaid program reimburses dentists just over 40% of what private dental insurance would pay for child dental services, compared to a national average of 66%.
A result is that of the 3 million kids eligible for dental services through Medicaid or the Children’s Health Insurance Program in Florida in 2023, only about 1.1 million received any care, while nearly two-thirds went without.
Why is Florida removing fluoride?

Most major dental associations and health organizations agree that when added to drinking water at recommended levels, fluoride is safe and helps strengthen teeth and prevent decay.
But Florida is the second state to ban communities from adding it to public water supplies. Utah became the first earlier this year.
When he signed the bill on May 15, Gov. Ron DeSantis pointed to studies that link consuming higher amounts of fluoride with negative side effects, including higher rates of attention deficit hyperactivity disorder and lower IQs in children. The levels of fluoride analyzed in those studies were twice the amount recommended for U.S. water supplies.
The ban, DeSantis said, is about giving families a choice.
“Yes, use fluoride for your teeth, that’s fine, but forcing it into the water supply is basically forced medication,” he said during a press conference in Dade City, a rural community north of Tampa.
Several places in Florida had already started removing fluoride from their water supplies amid concerns raised last year by state Surgeon General Joseph Ladapo and Robert F. Kennedy Jr., who at the time was President Donald Trump’s pick for U.S. Health and Human Services secretary. He was eventually confirmed.
Families can get dental benefits from fluoride in their toothpaste or by visiting the dentist for treatments, said DeSantis.
But for people struggling to meet basic needs, Cisneros, of Suncoast, said that’s not a given.
At the clinics, she said even some families who qualify for the lowest discount have a hard time paying for care.

“Some people will say, ‘But we’re talking about $25, why is it going to be complicated for somebody to come in and see a doctor with $25?’ But when you multiply $25 five times, because you have five kids, it becomes a burden,” she said.
Cisneros recalled working with families whose children share one toothbrush between them, or who use the same toothbrushes for a year as opposed to changing every few months, as is recommended.
The toothbrushes, she said, are “all bent and bad, you know in bad conditions, and they are still brushing with the same because they can’t afford simple stuff like that. Because it’s better to buy the milk or to buy, you know, the bread, than to buy a special toothbrush or special toothpaste.”
How oral health affects kids’ well-being
Dr. Michelle Thomas and other dentists said the impact of banning fluoride from drinking water goes beyond the trouble of maintaining healthy, attractive teeth.
“Children in pain can’t focus in school, they can’t eat properly, they can’t sleep — and oftentimes because of that, their guardians can’t sleep either and so it really affects the whole family,” said Thomas, a pediatric dentist and policy representative with the Florida Academy of Pediatric Dentistry.
Dental problems can also have emotional and economic tolls on children, said Dr. Frank Catalanotto, founding member of the advocacy group Floridians for Dental Access and former dean of the University of Florida College of Dentistry.
“It impacts academic performance, it impacts social development,” he said “The way out of poverty for a kid is education and if you can’t learn, you’re not going to get the best job.”

Children in rural areas have an especially hard time finding dental care. Dentists often cluster in Florida’s large cities where they can make more money, often seeking to pay off hefty student loan debts. The national average for a dentist is about $300,000.
Finding ones who specialize in treating children is another hurdle, said Thomas, who currently treats children, including those on Medicaid, in Panama City, located in Florida’s Panhandle.
Some families have to travel hours for appointments, she said.
“And so oftentimes their first visit to a dentist is because they’re having dental pain or a major dental issue that wills them to travel the long distance,” Thomas said.
Some families turn to hospital emergency rooms when they don’t know where else to go. In fact, the nonprofit CareQuest found in 2022, that children in Florida visited ERs for non-traumatic dental conditions at the highest rates in the country.
It’s a costly experience that doesn’t always address kids’ underlying issues.
“The emergency room legally must see you, they can’t turn you away, but the problem is no one in the emergency room is really equipped to handle dental problems,” said Catalonotto. “And so what [patients] get is antibiotics and pain medication, then they’re told to go see a dentist tomorrow. Well, if they couldn’t afford a dentist today, what they’re going to do is they’re going to get better for a couple of weeks and then the infection is going to come roaring back.”

Without fluoride, what’s next?
As evidence fluoride doesn’t work, some critics point to the fact that, despite its presence in many water systems, millions of Americans have untreated tooth decay.
But the Centers for Disease Control and Prevention — which considers community water fluoridation one of the greatest public health achievements of the 20th century — says adding it to water reduces cavities by about 25% in kids and adults.
Dr. Jeff Ottley, president of the Florida Dental Association, said ideally people should combine drinking fluoridated water with other dental care, such as using toothpaste and mouthwash.
“Without [fluoridation], it’s like driving in a car without air bags. You still have a seat belt, but you don’t have that air bag anymore,” he said.
Dentists interviewed for this story said fluoride isn’t the only solution to improving dental health. But they said removing it from water supplies will exacerbate a crisis in dental-care access that isn’t getting the attention it deserves.
“It will be even more important to have enhanced access to care, because I do anticipate that the number of cavities will increase significantly,” said Thomas.
State health officials say they are working to expand care.
Representatives of the Agency for Health Care Administration and Florida Department of Health declined WUSF’s requests to be interviewed for this story.
But in an email, the AHCA touted the Live Healthy Act Florida, passed in 2024, that raised Medicaid reimbursement rates for preventive dental services by nearly 59%. These include cleanings, sealants and fluoride treatments.
The agency added that the state’s Medicaid managed care plans “have the ability to cover services that go beyond the standard Medicaid fee schedules and coverage policies.”
The health department did not respond to questions about the fluoride legislation, but it shared a link to a program the state recently expanded that offers student loan repayment to dental professionals working in underserved areas.
The department also partners with community health centers like Suncoast to provide routine care in Title I schools, which provide additional support for students in low-income households.

But dentists said in interviews that more needs to be done to help kids who already have damage, regardless of their families’ immigration status or ability to pay.
They suggest increasing Medicaid payments for complex procedures so children with the greatest needs can get care as safely and comfortably as possible. To expand the workforce, they recommend helping other types of dental professionals get jobs and provide more incentives for dentists to work in rural and low-income communities.
It’s a tough demand in a climate of rollbacks. The U.S. Congress is considering cutting Medicaid, which could hamper states’ abilities to finance their own programs and strain community health centers already struggling to meet demand.
But dentist Tianna Wallick said kids need more care — not less.
“Because we traumatize children, essentially, when they’re put in these situations that, you know, they didn’t put themselves in,” she said.
This story is part of “Uninsured in America,” a project led by Public Health Watch that focuses on life in America’s health coverage gap and the 10 states that haven’t expanded Medicaid under the Affordable Care Act.